Complications & Prevention Of Urethral Strictures
Home > Urethral Stricture > Complications & Prevention Of Urethral Strictures
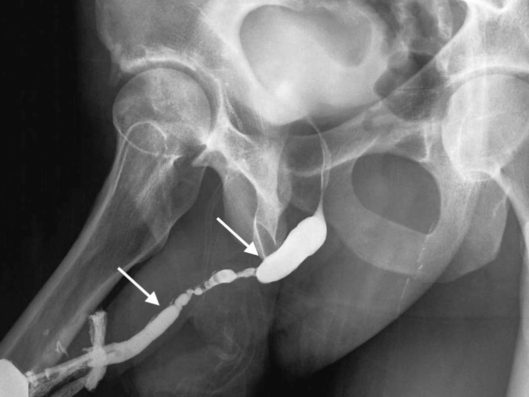
There was no imaging before this procedure, and therefore it can’t be determined if this was a short stricture that was made considerably longer as a urethrotomy complication or if the stricture was a 5-cm long stricture before treatment, and the patient was not aware of alternatives or the fact that the cure rate of urethrotomy for a stricture with that length and appearance is approximately zero.
The best data comes from Dr. A. Horiguchi in Japan. In Japan, Urologists are more likely to do urethral imaging before providing treatment providing a basis for comparison of the stricture length before the surgery and after surgery when there is a recurrence.
This published study nicely describes how these transurethral treatments (dilations and internal incisions from within the urethra) generally make the problem worse in the long run, and complicate the urethroplasty surgery needed for definitive repair.
Other complications of dilation and internal urethrotomy include major bleeding, false passage, and infection, and even rectal injury.
When instruments are advanced into the urethra blindly to stretch or tear the stricture open, the tip of the instruments (often metal rods of increasing size) may go into the wrong space, and as this wrong space gets dilated, a false passage is created. In some cases, if the urethra is torn clear through, there can be bleeding into the tissues surrounding the urethra causing scrotal swelling. In rare cases, the rectum can be punctured.
In an effort to reduce these false passage and perforation risks, Dr. Gelman developed a balloon dilator in 1999 that can be more safely used to dilate-tear the urethra open under direct vision. It was published on the cover of the Journal of Endourology in 2011.
Although this dilator makes urethral dilation safer, we never suggested it offered a higher long-term success rate compared to other dilation or incision methods.
The Importance of Finding a Stricture Surgery Specialist
At the Center for Reconstructive Urology, we exclusively specialize in urethral stricture and related male genital surgery, and our expertise and experience results in relatively few complications following surgery and usually very little post-operative pain. This level of success has led to many of our patients arriving as a referral from several hundred different Urologists over the past 20+ years. Most of these local urologists are certified to perform urethral reconstruction along with all other Urological procedures such as prostate cancer surgery, Female Urology, kidney stone surgery and other procedures involving the urinary tract. However, they refer their patients to our Center because they believe surgical success is best achieved at The Center for Reconstructive Urology with Dr. Gelman, a fellowship-trained sub-specialist whose practice is exclusively devoted to male urethral-genital reconstructive surgery.
Insurance Can Redirect Patients to Unqualified Urologists
In some cases, patients have been referred to us only to find The Center for Reconstructive Urology is out of their insurance network. Contrary to the wishes of the referring Urologist, the insurance company redirects the patient to a different in-network Urologist that is willing to attempt the repair. While it is reasonable for patients to be redirected if the motivation is to find a doctor more qualified, these decisions are usually made by insurance companies with little understanding of urology. The main goal of the redirection is to seek a physician and institution who will accept the patient at the lowest available rate.
In every case where patients have been redirected, it has not been to a Urologist more qualified based on training. In fact, patients are usually redirected to doctors who do not specialize in male urethral and genital reconstructive surgery and only perform the surgery part-time. Unfortunately, redirected patients usually tend to have failed outcomes and urethral stricture complications that can lead to disastrous results. Only after stricture surgery complications occur are the patients redirected to us, this time with insurance authorization, for complex re-do surgery. What most reinforces the fact that expertise makes a major difference in the outcome, is when our patients are referred to our Center with problems where our published success rate is 100% short term and 99.3% long term, have failed surgery, then have approval to have re-do surgery at our Center that is successful, but with a more complicated surgery. These unfortunate men have to undergo 2 major surgeries instead of one. https://www.centerforreconstructiveurology.org/video-library/insurance-complication/
Positioning-Related Stricture Surgery Complications
Certain urethral stricture repair surgeries require that the patient be placed in the lithotomy position, a position in which both legs are raised in the air in stirrups. More specifically, bulbar and membranous stricture repair (strictures underneath the penis) requires the patient to be in the lithotomy position, as the surgery is generally performed through an incision in the perineum, the area under the scrotum. If a patient is in the lithotomy position for an extended period of time, it is not uncommon for the top of their feet to experience numbness or tingling. This is not a significant problem if normal sensation returns sometime between 1 and 2 days, but a very prolonged sensation change is a cause for concern. Several of our patients have experienced this complication that eventually resolved, most of whom came into our center with complex strictures following a prior surgery that required extensive re-do reconstruction.
More serious positioning-related urethral stricture surgery complications include damage that affects foot or other leg movements. One such complication is called compartment syndrome. Compartment syndrome is when there is prolonged compression of the calves, leading to a build-up of pressure within the lower leg. This is considered a surgical emergency and must be treated immediately. Treatment consists of making deep, long incisions in the legs (called fasciotomies) to relieve the pressure.
To date, the Center for Reconstructive Urology has not had a single patient experience this positioning-related urethral stricture complication. However, we have seen patients who have reported a history of prior stricture surgery complications from poor positioning, including compartment syndrome or nerve damage that required them to use a walker or a wheelchair at the time of discharge.
We believe that the use of special equipment, along with careful attention to detail during positioning, can significantly reduce the risk of these complications. It is this cutting-edge equipment and extreme attention to detail that has led to our success with lithotomy positioning. At UC, Irvine Medical Center, all urethral reconstructive surgeries are performed using a Custom Skytron 6000 OR Table with a Jordan modification (as shown in yellow) to allow pelvic tilt.


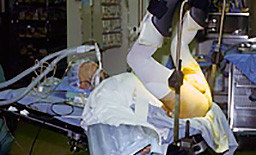
This table is designed specifically for urethral reconstructive surgery. As the pelvic portion tilts, the legs are proportionally raised. This prevents leg or hip flexion while simultaneously providing the pelvis with adequate support. Our stirrups are also custom modified according to Dr. Gelman’s preferences, allowing for the additional extension needed to further prevent excessive hip or knee flexion. The table’s unique design combined with the use of Dr. Gelman’s custom made stirrups means that no pressure is placed on the patient’s calves, and great care is taken to prevent pressure points.
We also try to minimize the time a patient is in the lithotomy position. For example, if a graft from inside the cheek (buccal mucosa) is required, this graft is harvested with the patient lying flat before placing them in the lithotomy position.
Erectile and Ejaculatory Dysfunction
It has been reported that after urethral stricture surgery, there can in some cases be sexual dysfunction such as decreased erection rigidity. Fortunately, when this urethral stricture surgery side effect occurs, there is resolution within 6 months. We closely monitor and document urinary and sexual function after surgery always seeking to make technical modifications to minimize risks, with one technical modification presented at the Annual Meeting of the American Urological Association in 2019. We have found that the specific techniques we use are associated with the least possible risk.






