PENILE AND SCROTAL SKIN DISORDERS, MAJOR PENILE INJURIES, FREE FLAP PHALLOPLASTY
Trauma and diseases of the penile and scrotal skin can lead to skin deficiency. Examples include penile skin cancers that can be cured with removal of the involved skin leaving a defect that requires coverage, and an infection involving the scrotal skin called Fournier’s Gangrene that is treated with complete removal of the affected tissues, leaving the need for skin coverage. When there is a penile skin deficiency, often there is redundancy in other areas. For example, if there may be a deficiency along the mid shaft of the penis, but there may be redundant foreskin towards the head of the penis. In these cases we mobilize the skin where redundant (where there is extra) to provide coverage where the skin is deficient. Every effort is made to avoid grafting as skin grafts are not as supple and soft and elastic as normal penile skin. If there simply is not an adequate amount of penile skin available, we can achieve coverage using a skin graft from the thigh. When there is scrotal skin deficiency, if closure can not be achieved using available scrotal skin, then skin grafts also provide nice coverage.
Subsequent to circumcision, some men develop skin bridges that originate along the distal penile skin and cross the coronal sulcus of the glans penis and fuse to the glans penis. These are also called penile skin adhesions.
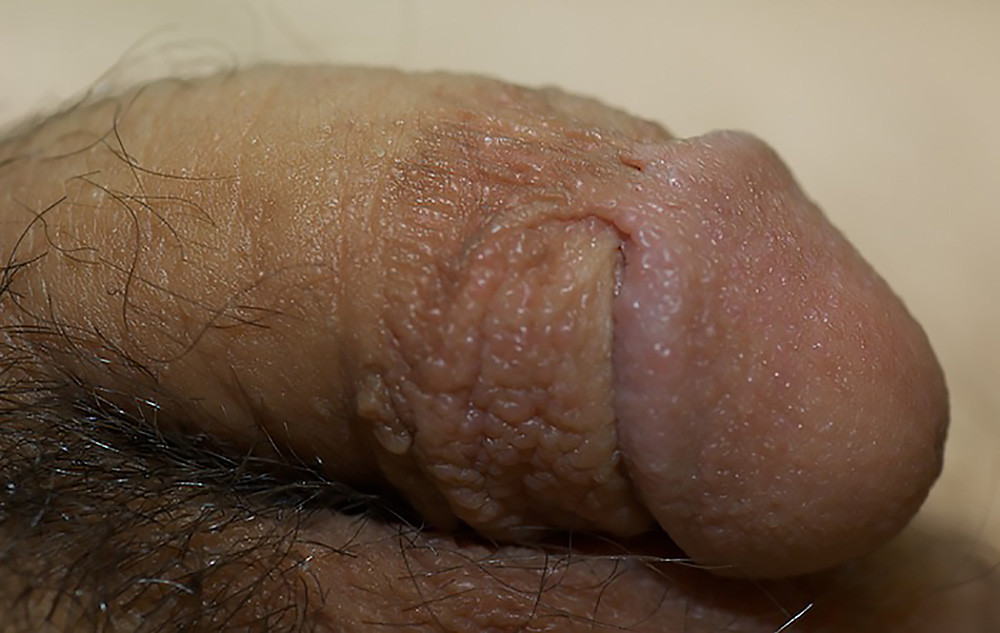
Penile skin adhesions in a 20 year old man.

Penile skin bridges. Note that these bridges cross over the coronal sulcus, the groove at the base of the penis. It is mentioned on internet discussions on this topic that with gentle retraction, these adhesions can be separated. However, in the above case, this would not be advisable. The only reasonable options are observation and incision of the bands with suture closure under local or other anesthesia. Treatment is not required, and observation is very reasonable. However, when these adhesions are associated with discomfort during sexual relations or of the patient finds the adhesions unacceptable, we offer treatment at the Center for Reconstructive Urology.
Causes of partial or total penile loss include partial or total penectomy, the surgical removal for a portion or all of the penis for the treatment of penile cancer (often squamous cell carcinoma of the penis). In addition there, can be penile loss as an infectious or ischemic (loss of blood flow) complication of penile surgery, which can be related to poor surgical technique by inexperienced surgeons. Moreover, there can be penile tissue loss from traumatic penile injuries.
In cases where the penis is severed with a sharp instrument such as a knife, and preserved, the penile can be re-attached surgically. When this is not an option, or then there is penile loss from other causes, the priority to to provide a patent urethral opening to allow the patient to urinate. When there is only partial penile loss with preservation of a stump, the patient can often effectively urinate while standing with the urethral opening placed at the tip of the remaining penis. When there is more complete loss, the urethral opening is often best created under the scrotum, a surgery called a perineal urethrostomy. The patient then must urinate while sitting, but this allows effective urination into the toilet.
One option to reconstruct a penis is called a phalloplasty, such as a forearm free flap phalloplasty. This is a major reconstructive surgery involving the use of forearm tissue that is transferred to the penile area, configured to be the shape of the penis, and re-attached using a microvascular surgery to re-establish blood flow and perhaps sensation. This can provide an appendage that may allow the patient to urinate while standing (with associated urethral reconstruction), and may provide the man the ability to have sexual penetration (with the insertion of a penile implant). However, there are significant limitations to this major surgery and patients considering this procedure must be carefully counselled. This surgery creates a phallus, not a “new penis” and the differences must be carefully explained before this surgery is considered.

