Urethral Stricture after Prostate Surgery or Radiation
Urethral stricture disease can occur as a complication of radical prostatectomy or as a side effect of radiation for prostate cancer. A blockage can develop where the bladder is connected to the prostate called a bladder neck contracture (also called bladder neck stenosis or urethrovesical stenosis). This area called the bladder neck can also become narrow from radiation related damage. Like a urethral stricture, a bladder neck contracture is a constriction or narrowing of that area, but since it is at the level of the bladder where the bladder meets the urethra, it is technically not called a urethral stricture. Furthermore, the treatment of a bladder neck contracture and a urethral stricture are different, and bladder neck contractures are discussed here.
When there is a narrowing of the actual urethra after radical prostatectomy (or surgery done through the urethra to treat an enlarged prostate, which is called a transurethral resection of the prostate or TURP) the most common location is near the tip of the penis. The technical term for that part of the urethra is called the fossa navicularis. A fossa navicularis urethral stricture is a complication of prostate surgery likely related to the urethral catheter or instrumentation that is required during and after prostate surgery. Although the catheter passes through the entire urethra, the fossa navicularis is particularly susceptible to narrowing This area of the urethra is at higher risk for stricture development when larger catheters are used, and this was a finding we previously published.
Fossa navicularis urethral strictures are not a common complication of prostate surgery. However, when there is a stricture, the narrowing is usually severe and not cured with dilation. Many of our patients come to us after being told they need to use a cone shaped plastic device to periodically stretch the tip of the urethra to keep it open as though there is no better alternative. Our preferred approach is to first evaluate the urethra with diagnostic testing including urethral imaging to determine the exact location of the stricture. If it is extremely short and very close to or at the tip of the penis, a very simple procedure called a meatotomy or extended meatotomy is curative. This is a surgery where the tip of the urethral opening is snipped open in the operating room and sutures are used on each side. However, if the stricture is longer, then the opening would be along the undersurface of the urethra was this surgery, and our preference for these strictures is a urethral reconstruction (also called a urethroplasty) using a small amount of penile skin (as a flap) as a patch to widen the narrow urethra. To date, we have had uniform success with this treatment, first published by Dr. Gelman’s mentor, Dr. Gerald Jordan.
After radiation therapy to treat prostate cancer with external beam radiation including “proton beam therapy” and/or radioactive seed implants, the most common location of a urethral stricture is the membranous urethra. This is the part of the urethra just under the prostate and the urethra in this area is surrounded by a muscle called the external urethral sphincter, which is one of the sources of continence. An illustration of the urethra showing the location of this part of the urethra is found here.
When patients are referred to the Center for Reconstructive Urology with blockage of urine flow after treatment for prostate cancer, they often are not clearly aware of their specific diagnosis with regard to the urethral stricture location and stricture length, even if they underwent prior treatment (such as dilation of the urethra) . If they only had a cystoscopy (looking inside the urethra with a scope) it is not possible to know the length of the stricture. If imaging was performed and that imaging did not include both a film during injection of contrast and during voiding (urination), there can’t be a definitive diagnosis.
We evaluate the urethra using both cystoscopy and high definition accurate urethral imaging to first determine the exact stricture length and location. This comes before a discussion of all options (which is never limited to dilations or self-catheterizations).
This is an example of a man who had radiation and was treated with numerous failed dilations without being aware that there were more effective alternatives until he was seen by a new Urologist who referred him to the Center for Reconstructive Urology. When we looked with a scope, the urethra was normal up to his membranous urethra, which was not unexpected. This confirmed that the stricture started at that portion of the urethra, but since the scope could not be advanced further, the urethral stricture length could not be determined. The following picture is a retrograde urethrogram (RUG) performed by Dr. Gelman.
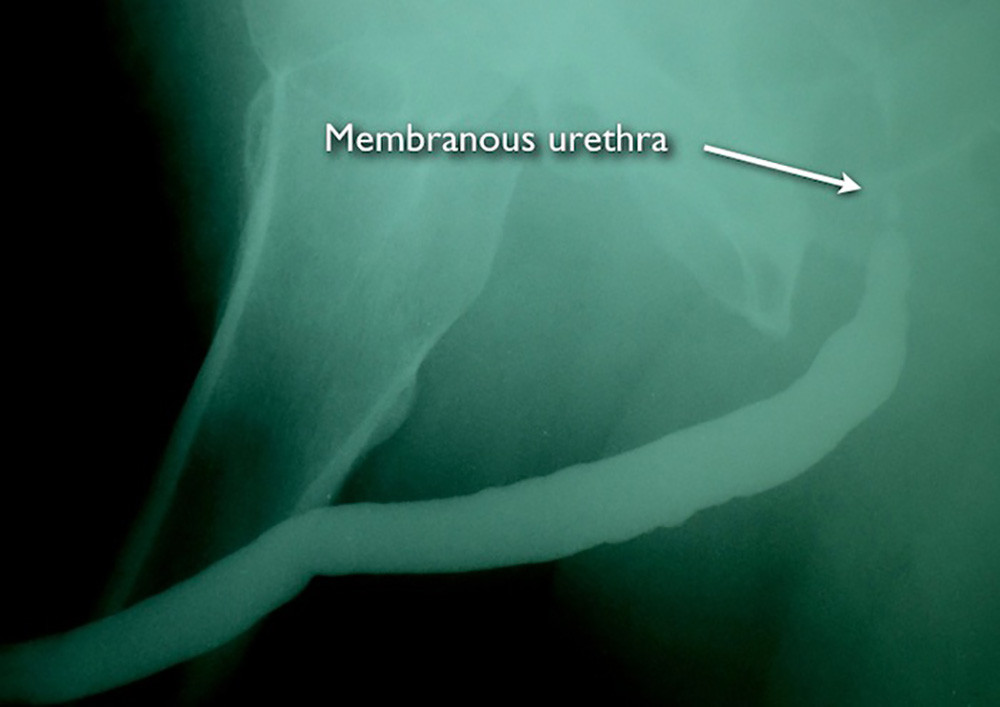
This is the retrograde urethrogram (RUG) of a patient with a membranous stricture. This study confirms a normal anterior urethra. This study does not diagnose narrowing of the membranous urethra because this portion of the urethra is normally closed when a patient is not urinating, and during a RUG, the patient is not urinating.
With the gentle injection of X-ray contrast to fill the bladder (a catheter should never be used for this purpose), we can then obtain a film during urination called a voiding cystourethrogram (VCUG)
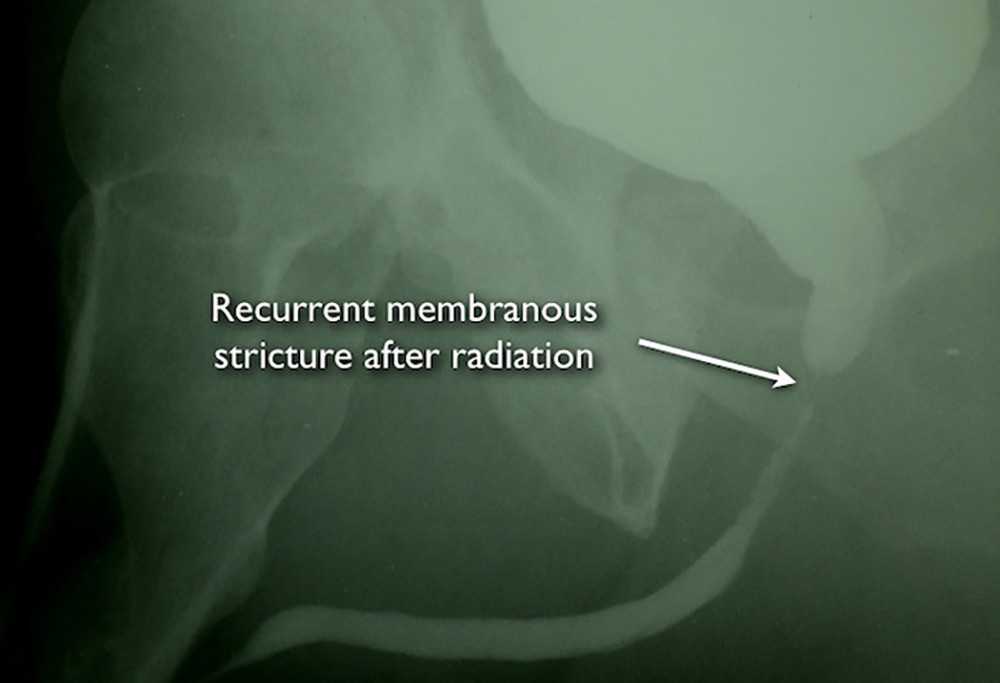
During urination with a bladder filled with X-ray contrast, the voiding cystourethrogram (VCUG) shows that the bladder neck opens normally. However, there is severe narrowing of the membranous urethra.
The voiding cystourethrogram confirms that the bladder neck and the urethra within the prostate itself are without any narrowing. When the information from the cystoscopy and imaging is taken together, it can be determined that there is urethral stricture narrowing of only the membranous urethra just under the prostate.
Treatment options include dilations and internal incisions. However, these are quick fix procedures generally only associated with temporary improvement of symptoms, and repeated dilations and incisions of stricture can make the stricture worse.
Fortunately, these strictures are highly amenable to posterior anastomotic urethroplasty, an operation that involves an incision under the scrotum under general anesthesia, the removal of the involved tissue, and a re-connection of the wide-open ends. Men with urethral strictures in the membranous urethra surrounded by the external sphincter are very concerned about developing urinary incontinence as a side effect of open urethroplasty surgery to treat the stricture. However, if the bladder neck is functioning normally, urine will stay in the bladder except during urination.
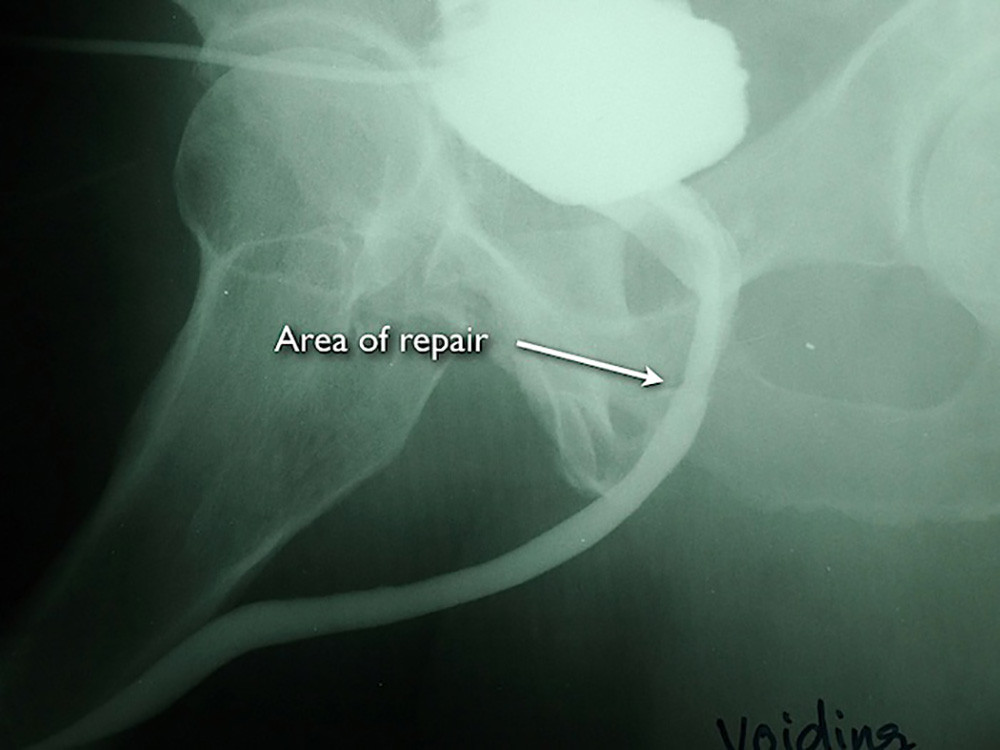
This is the VCUG after open repair, urethroplasty, with excision of the narrow area and reanastomosis. His surgery was 18 years ago, and his urethra remains patent without the need for dilations or other treatment.
The success rate of these surgeries is highly dependent on the skill and expertise of the Urologist performing this operation. We have seen patients whose Urologists attempt these surgeries and seem to have a 100% recurrence rate. This year, we reviewed our long-term outcomes with posterior urethroplasty for radiation urethral strictures involving the membranous urethra in patients who were compliant with long term follow-up (see table 1).
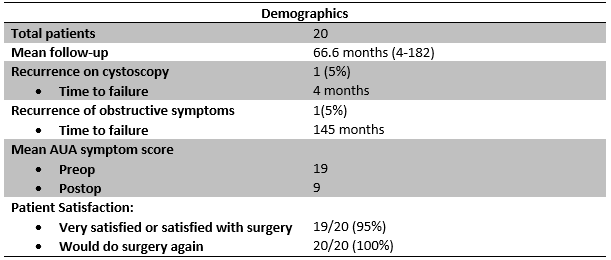
After surgery, our protocol is to look at the inside of the urethra with a cystoscope 4 months after surgery. This is done in our clinic without the need for sedation. We use a high-definition monitor to assess the urethra. Early success is defined as a urethra open enough that the size 16 French scope (16mm circumference) can pass through the area the repair easily. Only 1 patient had narrowing of the urethra at the connection to where the scope could not pass. However, the urethra was only very slightly smaller, the patient had no symptoms, and he did not require further treatment. In all other patients, the urethra was wide open.
We also monitor our patients for late recurrence with long-term followup given that we have 18 years of experience performing this and other urethroplasty surgeries (over 2,000 total cases). Only 1 patient developed some narrowing 145 months (12 years after surgery). One patient did develop some unanticipated incontinence and was not completely satisfied with the result. However, that patient and all other patients were asked “If you could do things over again, knowing what you know now about the result, would you still have the surgery?”. All of the patients (100%) said “yes”.
Our results should not be interpreted as a guarantee of success, but clearly prove that posterior urethroplasty, performed at the Center for Reconstructive Urology, generally offer our patients a cure and a markedly improved quality of life.

